Stop Guessing. Start Playing:
A Smarter Approach to Pickleball Injuries
dr. audrey falconi, do, RMSK
Pickleball has exploded in popularity across the Pacific Northwest.
It’s social.
It’s competitive.
It’s accessible.
And it’s easy to get hooked.
I have athletes playing up to six days a week.
With that growth, I’m seeing a steady increase in pickleball-related injuries in my Tacoma sports medicine clinic. The most common include:
- Knee pain — often arthritis flares or tendon overload
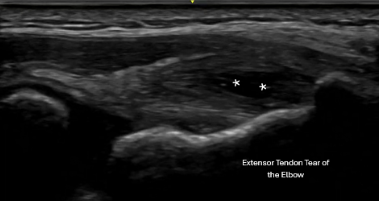
- Elbow tendinopathy (“pickleball elbow”)
- Calf muscle strains or partial tears — The most worrisome!
Pickleball demands lateral cutting, sudden deceleration, repetitive forearm loading, and explosive push-off. Over time, tissues break down when capacity doesn’t match demand.
But the biggest issue I’m seeing isn’t just the injury.
It’s what happens next.

The Cycle Many Pickleball Athletes Get Stuck In
Chronic pain.
Being told to “just rest.”
Being told to stop playing.
Delayed imaging or referrals.
Unsuccessful physical therapy.
Weeks turn into months. Rest DOES NOT rebuild tendon. Waiting DOES NOT restore tissue capacity and vague rehab without a clear diagnosis can target the wrong structure entirely.
Active adults don’t want to quit the sport they love.
They want answers — and a plan.
How Diagnostic Ultrasound Changes the Game
At Physician Coach, every evaluation begins with diagnostic ultrasound performed during your visit and BY THE PHYSICIAN who will be providing the treatment!
In-house results
Not ordered.
Not outsourced.
Not weeks later.
We examine your movement and visualize the tissue in real time.
In that same appointment, we determine:
- Exactly which structure is involved
- Whether it’s tendon, joint, or muscle
- The severity of tissue change
- Whether inflammation, degeneration, or partial tearing is present
This is the power of a Physician trained in Diagnostic Ultrasound.
From Diagnosis to Treatment in the Same Visit
If appropriate, treatment can begin immediately — in the same visit.
Using ultrasound guidance for precision, options may include:
- PRP (Platelet-Rich Plasma) for arthritis or partial tendon tears
- Prolotherapy
- Needle tenotomies to promote tendon healing
- Dry needling & Cupping therapy to treat supporting tissue
Because these treatments are guided in real time, they target the exact structure involved.
No blind injections.
No unnecessary delays.
No prolonged uncertainty.
This allows us to begin tissue healing right away — rather than waiting weeks to “see what happens.”

The Hip Is a Complex Joint
Hip pain can originate from:
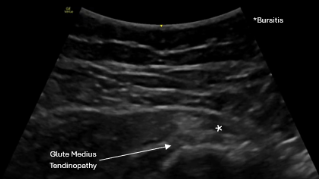
- Gluteus medius or minimus tendons
- Greater trochanteric bursa
- Rectus femoris tendon
- Hip joint (labrum or osteoarthritis)
- Proximal hamstring tendon
- IT band irritation
- Deep posterior hip structures
Symptoms overlap significantly.
Without imaging, lateral hip pain is often labeled “bursitis,” anterior pain is dismissed as tight hip flexors, and posterior pain is misattributed to the low back.
Ultrasound helps differentiate exactly where the pain and dysfunction are coming from — which completely changes treatment.
Beyond Pain Relief: Building Longevity in the Sport
Expedited diagnosis is only the first step.
Recovery must transition into performance.
We build:
- Progressive tendon loading
- Single-leg strength
- Lateral agility and deceleration mechanics
- Calf and foot resilience
- Load management strategies
The goal isn’t just returning to play.
It’s returning better, stronger, faster, and more resilient than before.
Play for the Long Run
Pickleball injuries don’t have to mean stepping away from the court.
With immediate clarity, precision-guided treatment, and a structured return-to-play plan, athletes can recover and continue playing the sport they love.
If you’re in Tacoma, Gig Harbor, Puyallup, or University Place and dealing with persistent pickleball pain —
Start with clarity.
Start with precision.
Start this week.